We have a definition problem in healthcare
By James W. Kim
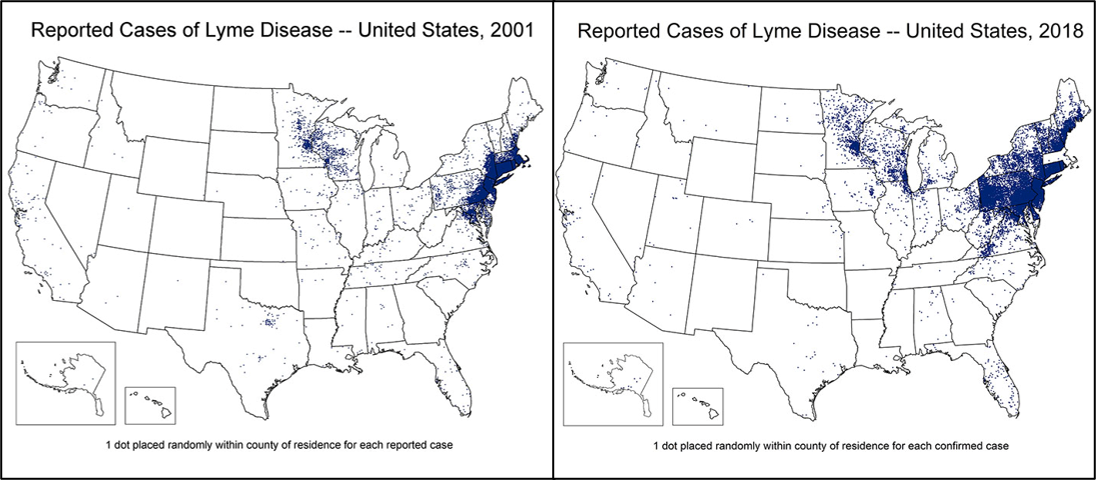
Advances in healthcare research and technology are messing with traditional definitions of diseases used in practice. This is a ticking time bomb.
It’s a problem that has bugged me for a better part of a decade, and it started in a hotel lounge during a medical device trade show somewhere in Southeast Asia (I think Kuala Lumpur). It was a cordial evening with drinks in the lounge with industry experts and physicians, and I was as green as I was eager to absorb all sorts of knowledge. The conversation, as they do when you corral these types, moved to major health issues. The topic of the night? Tuberculosis.
The TB Paradox
One of the physicians — a pulmonologist who had spent years working in Southeast Asian TB clinics — made a statement that stuck with me: “We don’t actually know how many people have TB.”
This was jarring. Tuberculosis is one of the most studied infectious diseases in history. The WHO publishes detailed annual reports. National surveillance systems track cases meticulously. How could we not know?
The answer lies in how we define “having TB.” The traditional definition relies on symptomatic presentation and confirmatory testing — sputum smear microscopy, culture, or more recently, molecular tests like GeneXpert. But these methods only catch active disease. Latent TB infection (LTBI) — where the bacteria are present but dormant — affects an estimated one-quarter of the world’s population. These individuals are not “sick” by traditional definition, but they carry a pathogen that can activate at any time, particularly if their immune system is compromised.
So do 2 billion people “have TB”? Or do only the 10 million who develop active disease each year “have TB”? The answer matters enormously for public health policy, resource allocation, and ultimately, the lives of millions.
Gonorrhea and the Definition Shift
The same definitional problem exists across many diseases. Take gonorrhea. The traditional definition focuses on symptomatic infection — urethritis, cervicitis, and their complications. Treatment guidelines are built around this definition.
But we now know that a significant proportion of gonorrhea infections are asymptomatic, particularly in women. These asymptomatic carriers can transmit the disease unknowingly, fueling ongoing transmission chains. Moreover, asymptomatic infections can still cause long-term complications, including pelvic inflammatory disease and infertility.
As diagnostic technology has improved — with nucleic acid amplification tests (NAATs) capable of detecting tiny amounts of bacterial DNA — our ability to identify asymptomatic infections has expanded dramatically. But our treatment guidelines, public health protocols, and disease definitions haven’t kept pace.
COVID-19 Made It Impossible to Ignore
The COVID-19 pandemic brought this definitional problem into sharp relief. Early in the pandemic, testing was limited to symptomatic individuals — those with fever, cough, and shortness of breath. By this definition, COVID-19 was a disease of the symptomatic.
But as testing expanded, it became clear that a substantial proportion of SARS-CoV-2 infections were asymptomatic or mildly symptomatic. These individuals were carrying and transmitting the virus without meeting the traditional “case definition.” The public health response — contact tracing, isolation, quarantine — was hampered by a definition that didn’t capture the full spectrum of infection.
Why This Matters
The gap between our evolving understanding of disease biology and our static definitions has real consequences:
Resource allocation: If we define diseases narrowly, we undercount them. Undercounting leads to underinvestment in prevention, diagnostics, and treatment.
Treatment guidelines: Clinical guidelines built on symptomatic definitions may miss the opportunity to treat — or at least monitor — asymptomatic individuals who are at risk of complications or transmission.
Public health policy: Screening programs, vaccination priorities, and surveillance systems all depend on how we define the diseases they target.
Diagnostics development: The IVD industry develops products based on clinical need as defined by current disease definitions. Broader definitions would create demand for different — often simpler, more accessible — diagnostic tools.
The Way Forward
We need a fundamental rethinking of how we define diseases in the age of molecular diagnostics and our growing understanding of pathogen biology. This means:
- Moving from symptom-based to pathogen-based definitions where appropriate
- Developing tiered definitions that distinguish between infection, latent disease, and active disease — each with appropriate management protocols
- Investing in population-level screening tools that can operate at scale and low cost
- Updating clinical guidelines to reflect the full spectrum of disease, not just its most obvious presentations
The ticking time bomb is this: as our diagnostic technology continues to improve, the gap between what we can detect and what we act upon will only widen. Every asymptomatic infection we choose not to define as “disease” is a missed opportunity for intervention — and a potential source of ongoing transmission.
We have a definition problem in healthcare. It’s time we started solving it.