A Case For The Perfect Healthcare System (for now)
By James W. Kim

Much like everything else in life, striking a careful balance is the only way to deliver sustainable healthcare to those who need it - which is everyone with a pulse. Nobody is exempt from being a stakeholder of this fundamentally human issue.
The Two Camps
The healthcare debate tends to polarize into two camps: those who advocate for fully socialized, government-run healthcare systems, and those who believe free market mechanisms are the only way to drive innovation and efficiency. The truth, as is often the case, lies somewhere in between.
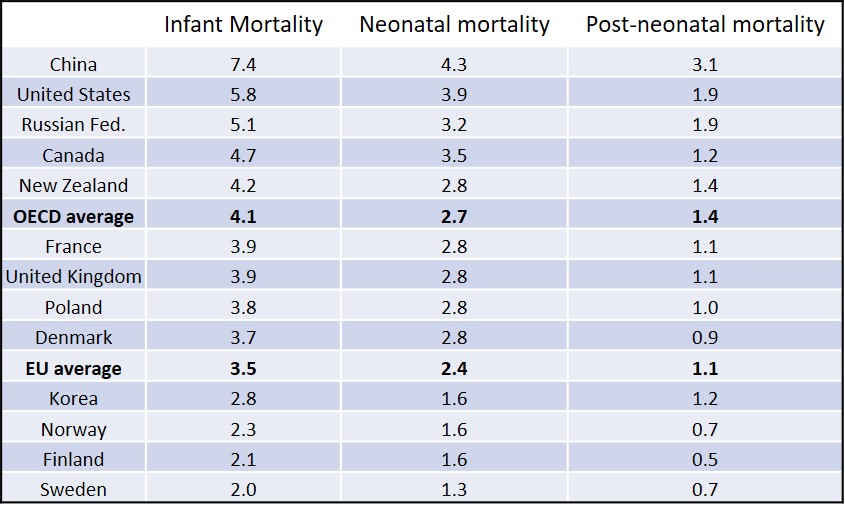 Chart 1: Infant, neonatal and post-neonatal mortality across OECD countries. Source: OECD Family Database
Chart 1: Infant, neonatal and post-neonatal mortality across OECD countries. Source: OECD Family Database
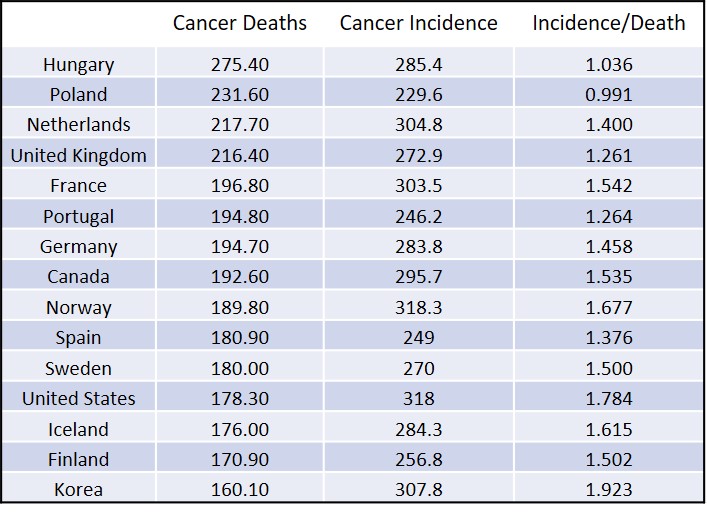 Chart 2: Cancer deaths and incidence per 100,000 persons. Source: OECD Health Status Data
Chart 2: Cancer deaths and incidence per 100,000 persons. Source: OECD Health Status Data
Proponents of fully socialized medicine point to countries like the UK (NHS) and Canada as models of universal coverage. And indeed, these systems have achieved something remarkable: every citizen has access to healthcare regardless of their ability to pay. However, these systems also face chronic underfunding, long wait times, and — critically — a diminishing ability to incentivize pharmaceutical innovation.
Free market advocates, on the other hand, point to the United States as evidence that market-driven healthcare produces the world’s most innovative treatments. This is also true: the US pharmaceutical industry accounts for a disproportionate share of global drug development. But the US system also produces the most striking disparities in access, with healthcare costs being the leading cause of personal bankruptcy.
The Relationship Between Monies Potential and Innovation
There is an undeniable relationship between the potential for financial returns and the willingness of private capital to invest in drug development. The average cost of bringing a new drug to market is estimated at $1-2 billion, with a development timeline of 10-15 years. No rational investor will commit these resources without a reasonable expectation of return.
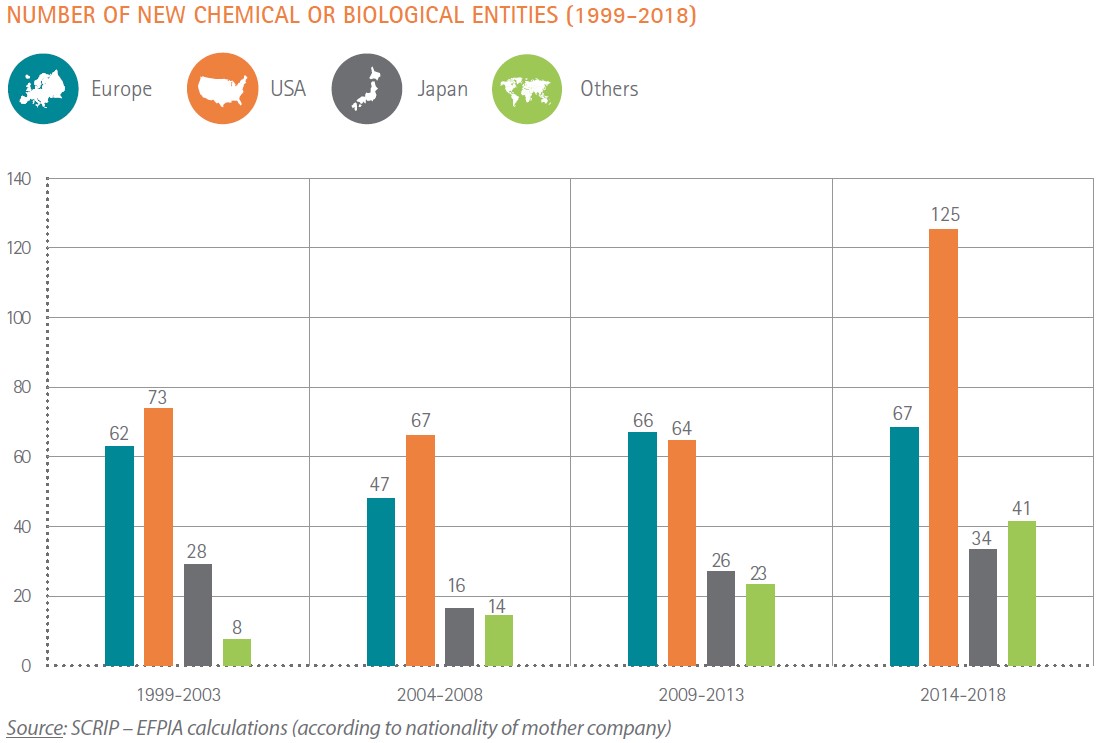 Figure 1: New chemical or biological entity introductions by country of origin. Source: EFPIA
Figure 1: New chemical or biological entity introductions by country of origin. Source: EFPIA
This is where OECD data becomes illuminating. Countries with the highest per-capita pharmaceutical spending also tend to be the earliest adopters of new therapies. This is not coincidental — it reflects the reality that pharmaceutical companies prioritize launches in markets where they can achieve pricing that justifies development costs.
Relationship Between Outcomes and Societal Health
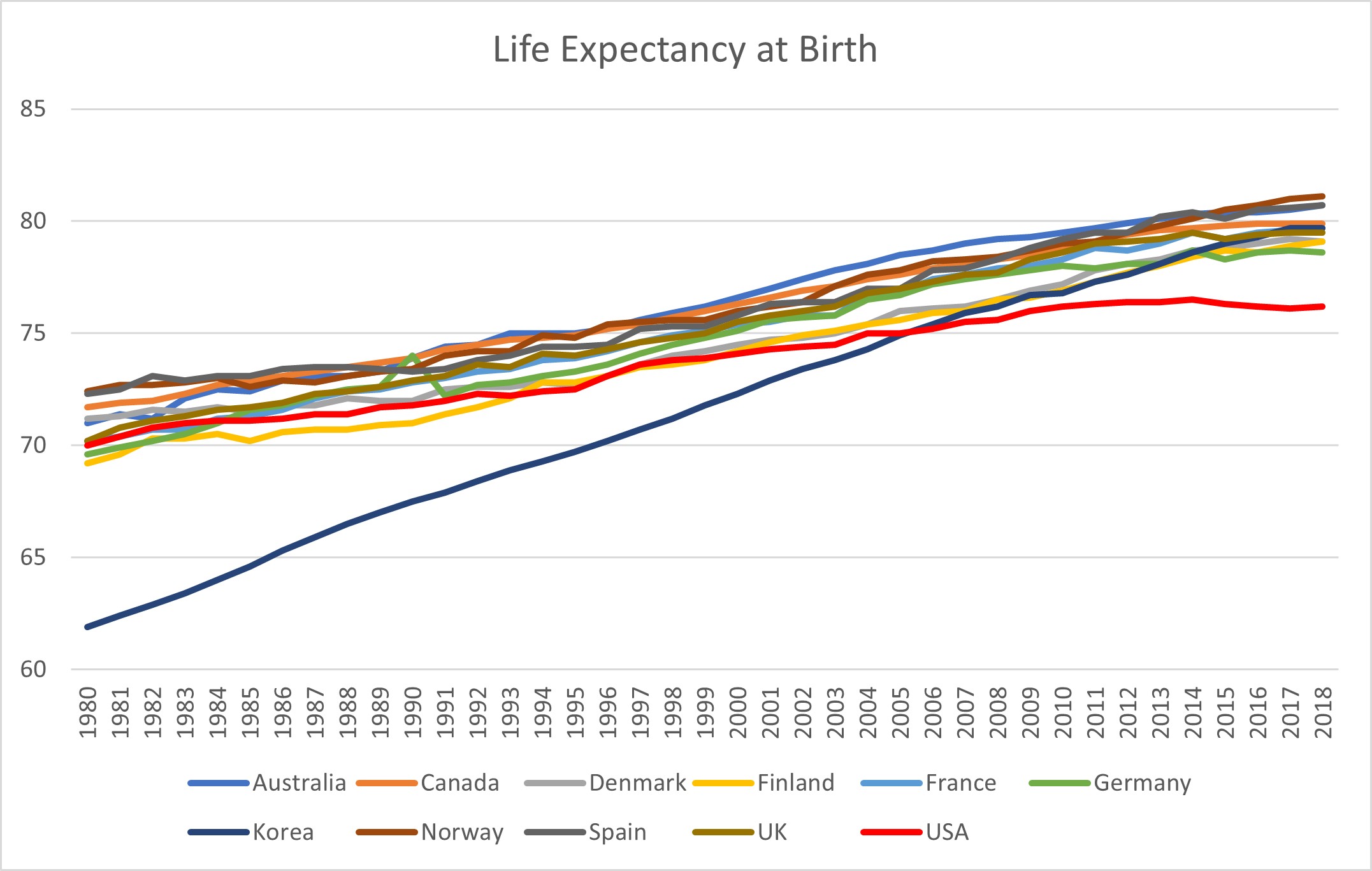 Figure 2: Life expectancy at birth of select OECD countries. Source: OECD Health Status Data
Figure 2: Life expectancy at birth of select OECD countries. Source: OECD Health Status Data
But money spent does not automatically translate to better outcomes. The US spends more per capita on healthcare than any other OECD nation, yet ranks poorly on many basic health metrics — life expectancy, infant mortality, preventable deaths.
This paradox suggests that the relationship between spending and outcomes is non-linear. There is a threshold below which spending cuts directly harm outcomes (as seen in austerity-affected healthcare systems), but also a point of diminishing returns above which additional spending primarily benefits narrow patient populations or enriches intermediaries rather than improving population health.
So What Are We Doing?
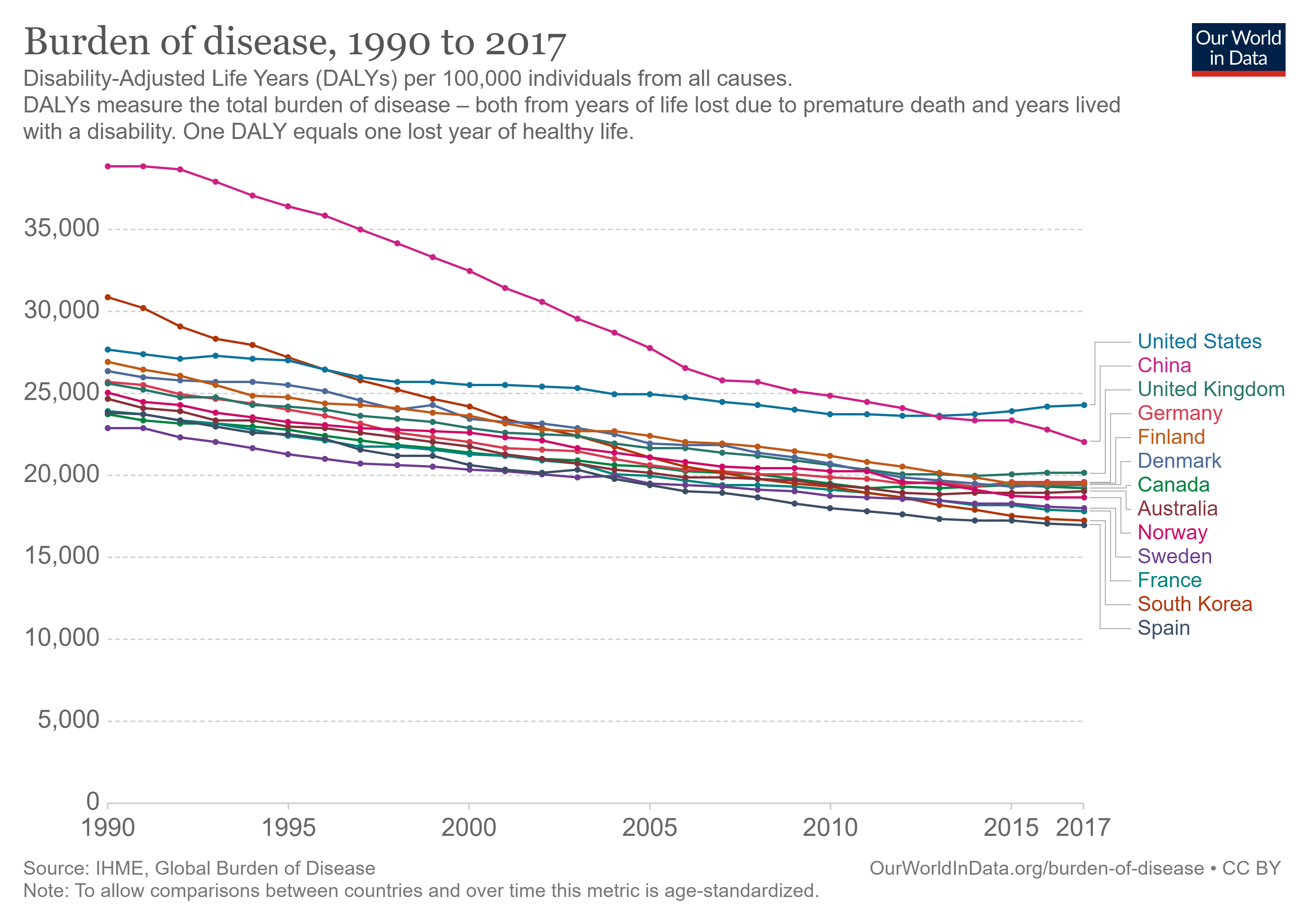 Figure 3: Burden of disease expressed as DALYs per 100,000 individuals. Source: Our World in Data
Figure 3: Burden of disease expressed as DALYs per 100,000 individuals. Source: Our World in Data
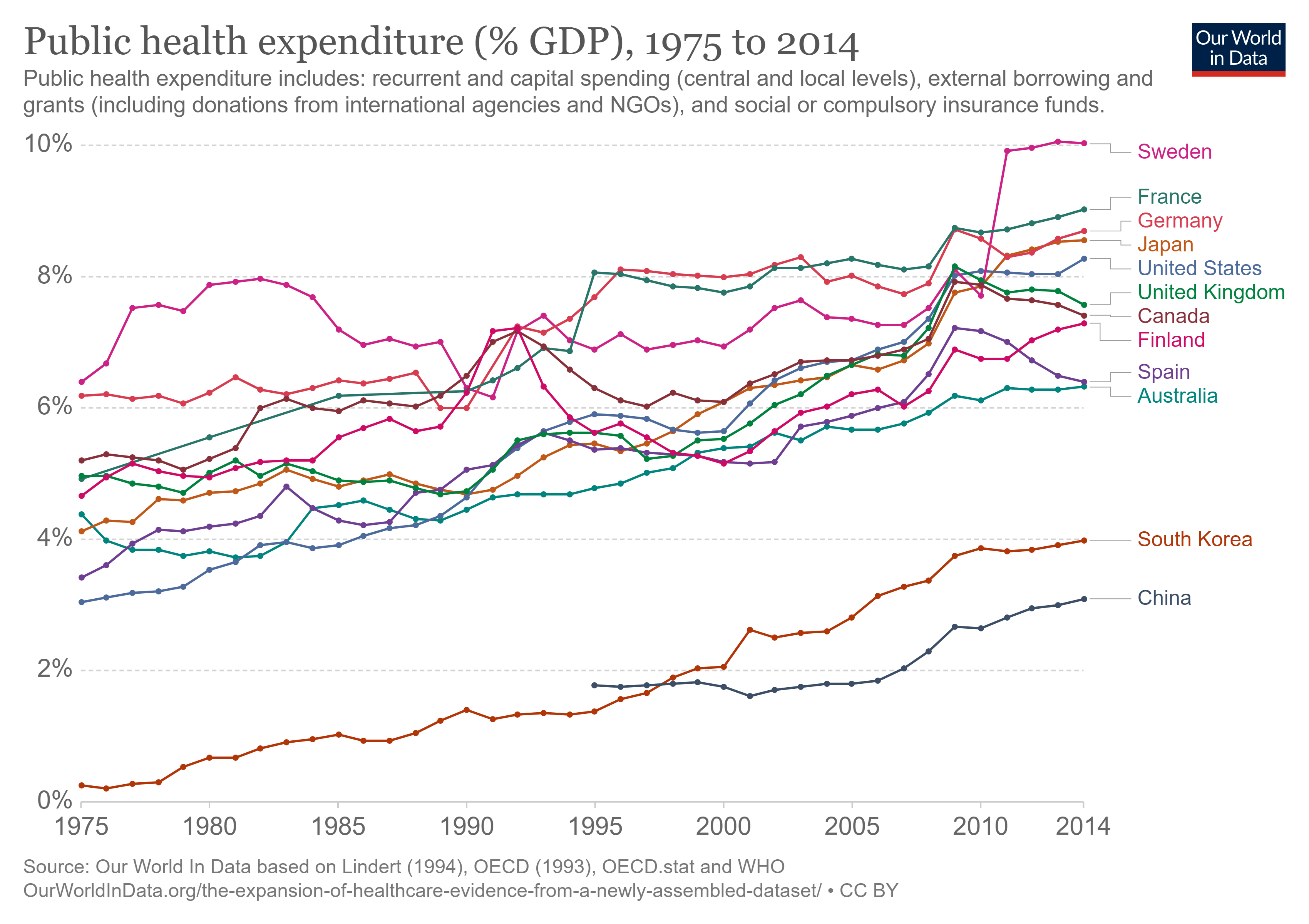 Figure 4: Public health expenditure as percentage of GDP. Source: Our World in Data
Figure 4: Public health expenditure as percentage of GDP. Source: Our World in Data
The current global approach to healthcare is, frankly, a mess. We have:
- High-income countries where pharmaceutical innovation thrives but access is increasingly stratified by income
- Universal systems that provide broad access but struggle to fund the latest innovations
- LMICs where even basic healthcare infrastructure is lacking, let alone access to advanced therapies
- Global health organizations that attempt to bridge these gaps through donation and subsidy models that create dependency rather than capability
The disconnect between those who develop medicines and those who need them has never been wider. And the COVID-19 pandemic has only amplified these disparities.
The Perfect Healthcare System?
Here’s a proposal, imperfect as it may be:
1. Universal basic coverage funded through progressive taxation. This covers primary care, preventive medicine, generic medications, and emergency care. Non-negotiable. Every human being deserves this baseline.
2. Patent-expiry-pegged expansion of universal coverage. As branded drugs lose patent protection and generics enter the market, these medications should automatically be incorporated into universal coverage. This creates a natural, economically sustainable pathway for expanding access to previously expensive therapies.
3. Maintained market incentives for innovation. During the patent period, pharmaceutical companies should be free to price their products according to market conditions. This preserves the financial incentives that drive innovation. However, transparency in R&D costs and pricing methodology should be mandatory.
4. Mandatory reinvestment in LMIC healthcare infrastructure. A small percentage of pharmaceutical revenues — not profits, revenues — should be directed toward building healthcare infrastructure in LMICs. Not donations, not charity, but genuine investment in manufacturing, training, and systems that create independent capability.
5. Outcome-based pricing for novel therapies. For truly innovative therapies, pricing should be tied to demonstrated patient outcomes. If a gene therapy claims to cure a disease, payment should be contingent on that cure being realized over a meaningful follow-up period.
Is this system perfect? No. Is it better than what we have? Almost certainly. The key insight is that healthcare is too important to be left entirely to the market, but too complex and resource-intensive to be managed entirely by governments. A hybrid approach that leverages the strengths of both — market incentives for innovation, public systems for access — is the only sustainable path forward.
The perfect healthcare system, for now, is one that acknowledges this tension and manages it thoughtfully rather than pretending it doesn’t exist.